|
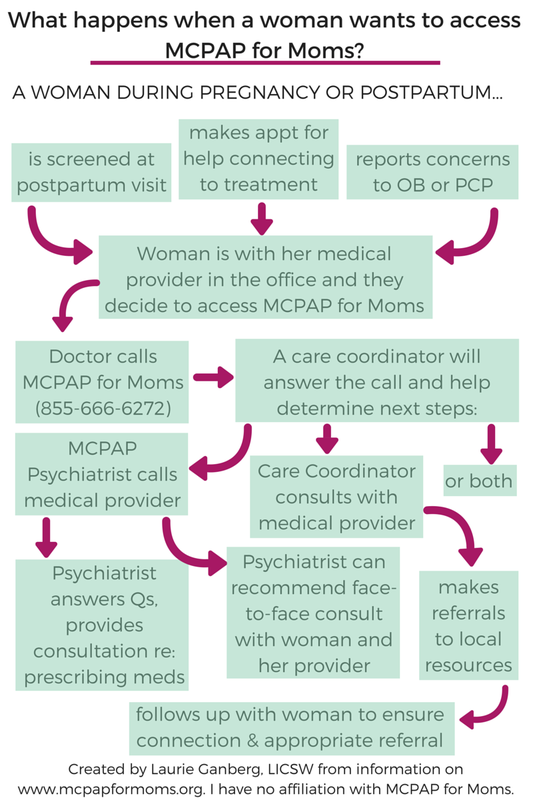
03/06/2015 UPDATE: I'm excited to share that Kathleen Biebel, PhD, Program Director for MCPAP for Moms (M4M) was kind enough to add some comments and clarifications to my post. I'm including her words below in red. And, they are working on creating their own infographic, which will aim to capture some more of the subtleties of the flow of what happens when a woman and her medical provider contact MCPAP for Moms. Once it's available, I'll be sure to link to it.  Another unique-to-Massachusetts resource, MCPAP for Moms offers medical providers a Monday-Friday 9-5 phone line to speak to a care coordinator who can connect the provider to a MCPAP for Moms perinatal psychiatrist for consultation and/or help with connecting a mother and family to a community perinatal mental health provider. What does this look like? If a woman is at her OB's office or is talking to her primary care provider (PCP), and she feels comfortable sharing that she is struggling with anxiety or depression or other emotional complications in the postpartum period, her doctor can call MCPAP for Moms. The medical provider will get a call back from a MCPAP for Moms psychiatrist to discuss diagnostic questions or get guidance about a medication prescription. (They can (and do) discuss a whole range of issues that can also include depression screening, community mental health resources – it can really run the gamut). A MCPAP for Moms care coordinator can also provide referrals for therapists and support groups in the woman's community who specialize in postpartum mood and anxiety disorders. Since finding psychiatrists that have openings, who feel comfortable managing medication in pregnancy or while breastfeeding, and who accept insurance can be an enormous challenge, there is the great potential for this to help with more rapid connection to treatment for moms. (Absolutely! Another huge part of what M4M docs do is to help the calling provider start and/or continue to provide mental health care for perinatal women when appropriate. This is a huge goal of M4M – to support OB and PCP and psychiatric providers as they attend to the mental health care of their patients, and to increase their capacity and comfort in doing so). My concern about the program, however, is whether it will be effective in increasing access treatment for women of color, who frequently experience discrimination in the medical system. I wonder whether women of color will be willing to bring their questions about emotional health to medical providers, especially if those providers have not already screened for emotional distress. I look forward to hearing more from MCPAP for Moms about who they're reaching. (We at M4M share your concern that minority and under-resourced women are more likely to experience perinatal mental health concerns, and are less likely to access and engage in treatment. M4M aims to increase access to treatment for all women by increasing the capacity of providers serving perinatal women with mental health concerns. Our M4M docs, when working with calling providers, encourage depression screening, discuss a wide range of treatment options and considerations, review community based resources, etc. Our M4M docs work with providers with the information they share with us about their patients, which may or may not address someone's racial or cultural identity. We at M4M do not provide any direct treatment for women). Medical providers who are looking for more information about MCPAP for Moms can look here. I've talked with many folks who are unsure how the MCPAP for Moms process works, so I created a little infographic to help explain it. The information was gathered at meetings I have been at with MCPAP for Moms and their website and represents my understanding of the program. I'm not affiliated with MCPAP for Moms. This post is part of the RESOURCES series where every week I feature websites, organizations, and information about perinatal emotional complications, parenting, therapy, reproductive health, and more. If you have a suggestion for a resource you'd like to see profiled, please let me know in the comments!  In 2007, Massachusetts implemented the Children's Behavioral Health Initiative (CBHI) in response to a class action lawsuit on behalf of Medicaid-eligible children with serious emotional disturbances to provide improved screening, evaluation, and access to behavioral health services for youth up to age 21 with MassHealth. One of the services created was Intensive Care Coordination (ICC) to "help get all the adults in your child’s life to work together." In my previous work as an in-home family therapist, mobile crisis intervention supervisor, and point of contact for families entering the CBHI system, I can tell you this is one of the biggest challenges and most important factors in providing effective care that wraps around and buoys a child and the family. While some families I worked with had a dedicated Intensive Care Coordinator, others relied on the family therapist or outpatient therapist to provide the coordination. Too often, it fell on a parent who was already approaching or well past the stage of burnout trying to decipher acronyms and navigate an incredibly complex system all while dealing with anxiety about finding help for their child. Throw in a doctor, a teacher, a special education services coordinator, an occupational therapist, or a mentor and it's not hard to imagine the benefit of making sure everyone's talking to each other. In my private practice, I see children and families, as well as individual adults, and I always consider who else is working with whoever is sitting with me in my office. Together, we review the pros and cons of signing releases allowing me to communicate with those other providers. Here are some common themes that arise:
One of my strengths is looking at the bigger picture and navigating larger systems. When we think together about who is currently involved in your life and how you'd benefit from working with other providers, we have the best chance of efficiently meeting your goals, but it's critical that appropriate communication happens to ensure everyone on your team is working together. Do you have any success stories or cautionary tales of collaboration among providers? Therapists, what makes you hesitant or excited to take on the role of coordinating care? Please feel free to share your thoughts in the comments. |
Therapy, Groups, Supervision, Consultation, Training in Seattle, WA and online in Washington state
Laurie Ganberg, LICSW, PMH-C (#LW60673320) ~ Specializing in Perinatal Mental Health, Trauma, & Fat Liberation
Now practicing through Fiddlehead Therapy, PLLC with online services and in person in Mountlake Terrace, WA
Home | Privacy | Contact | Zoom Link
© 2019-2024 All rights reserved
Laurie Ganberg, LICSW, PMH-C (#LW60673320) ~ Specializing in Perinatal Mental Health, Trauma, & Fat Liberation
Now practicing through Fiddlehead Therapy, PLLC with online services and in person in Mountlake Terrace, WA
Home | Privacy | Contact | Zoom Link
© 2019-2024 All rights reserved