|
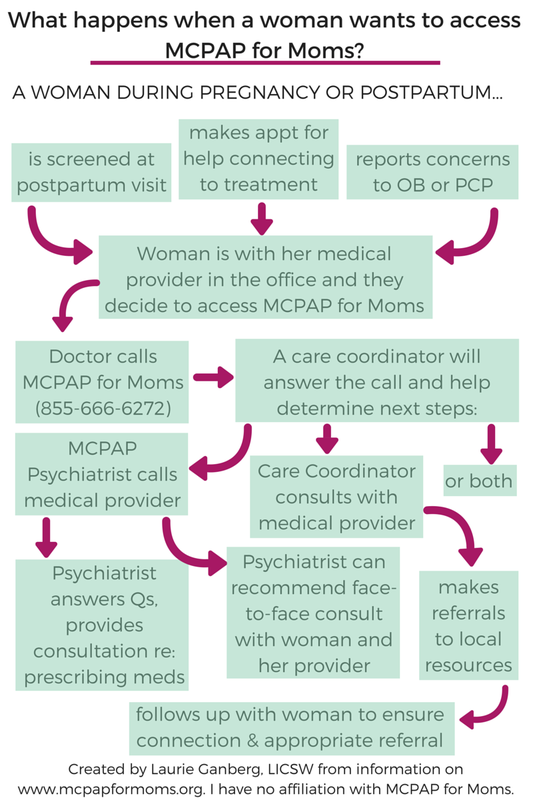
03/06/2015 UPDATE: I'm excited to share that Kathleen Biebel, PhD, Program Director for MCPAP for Moms (M4M) was kind enough to add some comments and clarifications to my post. I'm including her words below in red. And, they are working on creating their own infographic, which will aim to capture some more of the subtleties of the flow of what happens when a woman and her medical provider contact MCPAP for Moms. Once it's available, I'll be sure to link to it.  Another unique-to-Massachusetts resource, MCPAP for Moms offers medical providers a Monday-Friday 9-5 phone line to speak to a care coordinator who can connect the provider to a MCPAP for Moms perinatal psychiatrist for consultation and/or help with connecting a mother and family to a community perinatal mental health provider. What does this look like? If a woman is at her OB's office or is talking to her primary care provider (PCP), and she feels comfortable sharing that she is struggling with anxiety or depression or other emotional complications in the postpartum period, her doctor can call MCPAP for Moms. The medical provider will get a call back from a MCPAP for Moms psychiatrist to discuss diagnostic questions or get guidance about a medication prescription. (They can (and do) discuss a whole range of issues that can also include depression screening, community mental health resources – it can really run the gamut). A MCPAP for Moms care coordinator can also provide referrals for therapists and support groups in the woman's community who specialize in postpartum mood and anxiety disorders. Since finding psychiatrists that have openings, who feel comfortable managing medication in pregnancy or while breastfeeding, and who accept insurance can be an enormous challenge, there is the great potential for this to help with more rapid connection to treatment for moms. (Absolutely! Another huge part of what M4M docs do is to help the calling provider start and/or continue to provide mental health care for perinatal women when appropriate. This is a huge goal of M4M – to support OB and PCP and psychiatric providers as they attend to the mental health care of their patients, and to increase their capacity and comfort in doing so). My concern about the program, however, is whether it will be effective in increasing access treatment for women of color, who frequently experience discrimination in the medical system. I wonder whether women of color will be willing to bring their questions about emotional health to medical providers, especially if those providers have not already screened for emotional distress. I look forward to hearing more from MCPAP for Moms about who they're reaching. (We at M4M share your concern that minority and under-resourced women are more likely to experience perinatal mental health concerns, and are less likely to access and engage in treatment. M4M aims to increase access to treatment for all women by increasing the capacity of providers serving perinatal women with mental health concerns. Our M4M docs, when working with calling providers, encourage depression screening, discuss a wide range of treatment options and considerations, review community based resources, etc. Our M4M docs work with providers with the information they share with us about their patients, which may or may not address someone's racial or cultural identity. We at M4M do not provide any direct treatment for women). Medical providers who are looking for more information about MCPAP for Moms can look here. I've talked with many folks who are unsure how the MCPAP for Moms process works, so I created a little infographic to help explain it. The information was gathered at meetings I have been at with MCPAP for Moms and their website and represents my understanding of the program. I'm not affiliated with MCPAP for Moms. This post is part of the RESOURCES series where every week I feature websites, organizations, and information about perinatal emotional complications, parenting, therapy, reproductive health, and more. If you have a suggestion for a resource you'd like to see profiled, please let me know in the comments!  Recently, there was a blog post by a new mother about how amazing her experience of motherhood was: "They should’ve warned me that my life was about to become so rich and beautiful and fulfilling, that I’d look back on what it was before and think, “Poor me. I didn’t know her yet.”". Predictably, there were responses decrying the one dimensionality of her piece: "I'm biased, having found the experience of parenting wonderful AND hard." This media hubbub about what we should be telling pregnant women and expectant couples about the realities of parenthood illustrates the conundrum of educating parents. Everyone's experience of the early postpartum period is different, influenced by their own health; their support system; their baby's temperament; their family of origin and history; their socioeconomic and work situation; their cultural, racial, and ethnic background; and countless other factors. I've been mulling all this over with my Becoming Parents Workshops. How do I offer a workshop to prepare parents-to-be to face common challenges inherent in life with a new baby, without resorting to scare tactics, all while acknowledging that neither I - nor they - can know what their reality will be until they're actually living it? Stumbling blocks are common issues that can arise for new parents. Some new mothers will be able to gracefully step over one or all of them. Others will be tripped up momentarily. And a few will be brought to their knees. But, recognizing these stumbling blocks makes it easier to avoid falling over them & to stitch together a safety net for the family. Balancing Needs  A newborn is completely dependent on her parents for nourishment, comfort, care, even for help burping. Of course meeting her needs is the priority; yet, I'm going to employ the tired airplane oxygen mask metaphor and say that mothers need to take care of their own needs in order to be able to take the best care of their babies. And where does the partner figure into this scenario? He or she also needs to figure out how to take care of their own needs. Then, both partners can be mindful of taking care of each other and their relationship. When parents feel like they're functioning well as a team, they're better able to handle the challenges of meeting baby's needs. The challenge is finding time and energy, and understanding the other's experience. It's a process to learn how to do this - I can't give anyone a magic formula (though I would if I could!) - but when a family goes through this learning curve to balance everyone's needs, they'll also be better able to shift how needs are met over time as the baby grows and the challenges change. Practical suggestions: Hire a postpartum doula for extra help in the early months, make sure each partner has opportunities to take care of the baby solo to gain confidence and competence and let the other partner get out of the house, put the baby down in a safe place when he won't stop crying and take 5 minutes with headphones on, or in the shower, or out on the porch to breathe and regroup. Reconciling Reality and Expectations  Imagining life with the baby is one of the joys of pregnancy. But it's inevitable that there will be discrepancies between those dreams and reality. Understanding how often a newborn baby needs to eat (8 to 12 times in a 24 period) and why (because their stomachs are tiny - only the size of an egg by weeks 2-3!) can help parents-to-be realistically anticipate life with baby. I spend time in my workshops talking about breastfeeding basics so that both parents can be on the same page and I make sure parents know where to turn for help if they run into challenges feeding the baby. Plans about, wishes for, and the reality of maternity/paternity leave also often clash. In the US, there's a propensity to think about maternity leave as "vacation" and I often see new mothers trying to do too much while they should be healing, learning and bonding with their baby, and taking care of themselves. And thanks to our lack of paid family leave, partners are often lucky if they can take 1 week off, while most mothers that I work with cobble together 6-12 weeks using sick time, vacation, short-term disability, and unpaid time off. There are other families that realize after the baby is born that the cost/benefit analysis of daycare and work shakes out differently and plans they made during the pregnancy change. Practical suggestions: Pregnant women can usually attend breastfeeding groups; if you're planning on breastfeeding I recommend going once before you have the baby. You'll likely see women nursing their babies; hear about breastfeeding realities, pumping, and a few tips/tricks; and meet the leaders or facilitators of the group. A friend pointed out that she was much more likely to contact one of the counselors at a local breastfeeding group once she'd met them, rather than cold-calling with a problem in the early days of her baby's life. Again, a postpartum doula can help new parents understand typical newborn behavior, develop and bolster trust in those parental instincts, and be a resource for questions about your baby. Babies are constantly developing and changing. When you think you have it figured out, your baby's going to switch it up; and when you think you won't be able to handle your baby's challenging behavior anymore, your baby's going to switch it up. Remind yourself "this will change" (without any pressure to enjoy it!). The same applies to new parents: make plans as best you can, but anticipate that you and those plans might change. Hint: there's usually not just one "right" decision. The who/what/why/how of asking for help  The last stumbling block I want to talk about is the tension between wanting time to adjust to being a new family of ___, understanding extended family's desires to meet the baby, making sure no one becomes isolated, and asking for help. Of course these building blocks are all connected and, often, expectations and reality need to be reconciled about how family or friends will help once the new baby arrives. Challenges frequently arise in relationships with parents and in-laws - now "the grandparents." Becoming a parent can be a time to reflect about your own childhood and identify ways you want to emulate your parents or do things differently. You may be surprised by your own strong opinions about how family members act with the baby and may be uncomfortable expressing your wishes. Or you may find that others can't follow through with what you ask of them and disappointment or anger rises. When family relationships are complicated, they often become more complex with the changes in family roles. For expectant couples who have lost parents, grief can resurface during pregnancy, birth, and the postpartum. A note about isolation: It is very easy to become isolated in the postpartum period. There are many cultures that prescribe a period of time (often 30-40 days) that a new mom stays at home with the baby, but often in these cultures, they are being visited by extended family and community members who are helping, talking with them, and taking care of them and the home. In the US, we have neither the cultural expectation that a new mother stay at home for a period of time, nor do we have the systems of support (visiting nurses, close family, family leave) that other countries and cultures create for new families. So parents-to-be are often left to build community around their new family, utilizing paid help when possible, friends/family/neighbors when available, and local formal and informal groups of other new parents. Practical suggestions: Spend some time during the pregnancy preparing a postpartum plan. We do this in my Becoming Parents Workshop. At a minimum, include specific information about local breastfeeding and new parent groups along with a plan for help with meals. Ask a friend or family member to set up a meal train (there are many, free options). On the baby registry, ask for an Instacart membership or other grocery delivery service. Once again, a postpartum doula can be a valuable additional support for those families that can afford to hire one - another thing to think about including on a registry if it's outside your means. Lastly, be aware of the signs of postpartum emotional distress and how the baby blues differ. If you find yourself or your partner struggling, please reach out for help. Postpartum Support International has an English and Spanish warmline available, or contact me.  I've written before about why I think support groups are helpful. This resource is an informational flyer about four of the postpartum support groups in the Boston area. There are other groups that are run periodically by individual providers and other groups further afield. I find that with my practice in Cambridge and the work I do in Concord, these are the ones that I'm continually referring to, so I thought I'd make an easy flyer to share. I hope that lactation consultants, doulas, other therapists, OBs, midwives, childbirth educators and any one else that works with pregnant or postpartum women might share it with their clients so that if a new mom needs a group for support in the postpartum period with postpartum depression, anxiety, or general adjustment stress and challenges, they'll know where to turn!
 The PPD Awareness Day organized by the Massachusetts Legislature's Special Commission on Postpartum Depression, entitled Bringing Postpartum Depression Into the Light: Decreasing Stigma, Supporting Families, and Implementing Policy Change in Massachusetts, has been postponed due to the latest snow. As soon as it gets rescheduled, I'll share the news here.  I've been doing some volunteering for Postpartum Support International of MA so I'm especially eager to share that we have been updating the provider and support group listings available on the PSI of MA website or by calling their warmline at 1-866-472-1897. What's a warmline you ask? You call and leave a message and within 24 hours, a volunteer will get back to you to answer questions about postpartum depression, anxiety, and other adjustment challenges, as well as help connect you to providers and support groups in your area. If you're troubled what you or a family/friend is experiencing in the postpartum period and don't know where to start, the PSI of MA warmline is a great place to turn to talk to a knowledgeable, supportive trained volunteer. This post is part of the RESOURCES series where every Thursday I feature websites, organizations, and information about perinatal emotional complications, parenting, therapy, reproductive health, and more. If you have a suggestion for a resource you'd like to see profiled, please let me know in the comments! |
Therapy, Groups, Supervision, Consultation, Training in Seattle, WA and online in Washington state
Laurie Ganberg, LICSW, PMH-C (#LW60673320) ~ Specializing in Perinatal Mental Health, Trauma, & Fat Liberation
Now practicing through Fiddlehead Therapy, PLLC with online services and in person in Mountlake Terrace, WA
Home | Privacy | Contact | Zoom Link
© 2019-2024 All rights reserved
Laurie Ganberg, LICSW, PMH-C (#LW60673320) ~ Specializing in Perinatal Mental Health, Trauma, & Fat Liberation
Now practicing through Fiddlehead Therapy, PLLC with online services and in person in Mountlake Terrace, WA
Home | Privacy | Contact | Zoom Link
© 2019-2024 All rights reserved